Widespread HPV vaccination could significantly reduce the frequency of cervical cancer screenings, according to new research from Norway. The study suggests that women vaccinated between ages 12-24 may only need screenings every 15-25 years, while those vaccinated later (25-30) could extend intervals to a decade. This is a major shift in how cervical cancer prevention could work in countries with near-universal vaccination.
The Norwegian Model: Vaccination and Screening Combined
Researchers used mathematical modeling to determine optimal screening schedules based on high HPV vaccine coverage (over 90% in Norway as of 2021) and a consistent screening program. Norway utilizes HPV testing every five years, which is more effective at detecting precancerous cells than traditional Pap tests. Their strategy is so successful that projections suggest they could eliminate cervical cancer by 2039.
The HPV vaccine is a cancer-preventing tool, proven safe and effective. When administered early, it creates long-term protection, reducing the need for frequent checkups.
Why This Matters: HPV and Cancer Risk
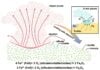
Human papillomavirus (HPV) is a common sexually transmitted infection. Most infections clear on their own, but persistent high-risk strains can lead to cervical, throat, penile, and anal cancers. Vaccination prevents infection, while screening detects existing cases. The key takeaway is that high vaccine coverage changes the risk profile, making less frequent screenings viable.
US Context: Vaccination Gaps and Screening Declines
The United States lags behind Norway in HPV vaccination rates (around 57% for 13-15 year olds as of 2023). Screening consistency is also a challenge: roughly a quarter of women aged 21-65 were overdue for cervical cancer screening in 2023, with rates still recovering from pandemic-related dips.
“The conditions in Norway… differ from the situation that we are in, in the United States,” explains Kimberly Levinson of Johns Hopkins Gynecologic Oncology.
This means that while the Norwegian model is promising, it is not directly transferable. The US must prioritize increasing vaccination rates and improving screening adherence before reducing screening frequency.
The Bottom Line
The study highlights the potential for streamlined cervical cancer prevention in well-vaccinated populations. However, both vaccination and consistent screening remain crucial in countries like the United States, where HPV coverage is incomplete and screening rates are falling. Promoting both strategies is essential to maximizing protection.